In an attempt to head off burnout, I began documenting my clinical interactions in a separate notebook in order to search for patterns and deficits in my skills or clinical reasoning. After months of doing this, I was able to identify some patterns in my thinking and take a more systematic approach to the patient interview process. After discussing this with my mentor, he recommended this APTA short course for its focus on self-reflection and personal growth.
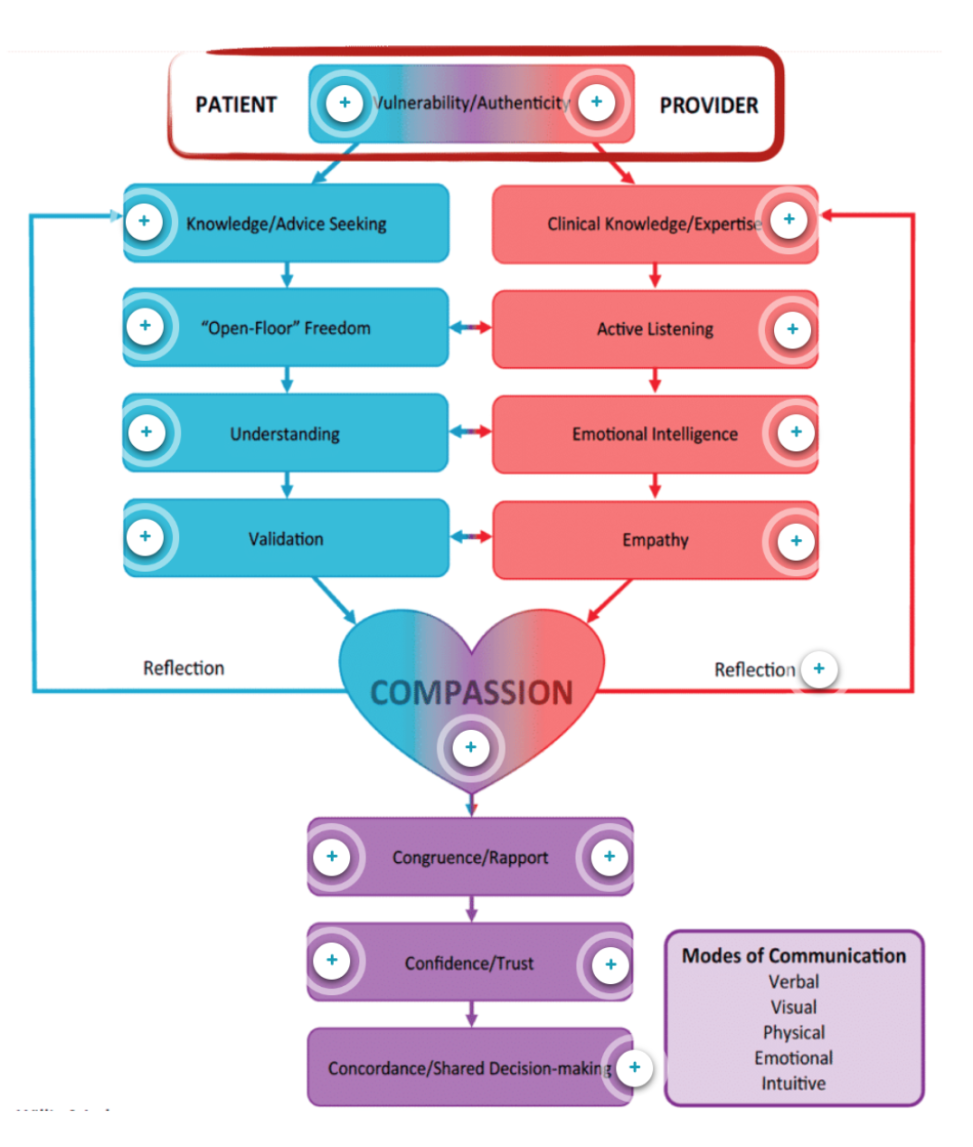
What resonated with me most was the idea that compassion and deep connection can actually prevent burnout. Researcher Brené Brown, featured as part of the APTA’s Compassionate H.E.A.R.T. model, emphasized that “boundaries are a prerequisite for compassion and empathy.” This insight left a lasting impression, shaping not only my clinical practice but also my personal life. The model’s focus on vulnerability, authenticity, and active listening also resonated with me, though not to the same extent.
By fostering meaningful connections and maintaining an open and empathetic approach, I feel able to navigate the challenges of clinical practice while preserving my own mental and emotional health. The course’s emphasis on continuous reflection and adaptability aligns with my commitment to clinical excellence and delivering thoughtful, patient-centered care.